Diabetes Eye Disorders
Diabetes is a disease that affects all areas of your body—including your eyes. Eye care is especially important for people with diabetes, because they are at an increased risk of developing eye complications from the disease. In fact, diabetes is the leading cause of blindness in adults age 20 to 74.
- Unfortunately, most people with diabetes will get some form of retinopathy, a disorder of the retina.
- The earlier problems are diagnosed, the more successful the treatments can be.
What is diabetic retinopathy?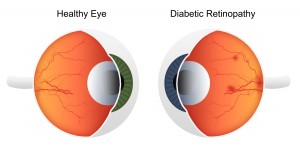
Diabetic retinopathy is a disease of the small blood vessels that nourish the retina. It is especially prevalent in Type I or insulin-dependent diabetics. In some cases, blood vessels weaken and can begin to leak fluid, fatty or protein deposits, and blood, reducing the nourishment to the retina. The longer you’ve had diabetes, the more likely you are to have retinopathy. Almost everyone with type 1 diabetes will eventually have nonproliferative retinopathy. And most people with type 2 diabetes will also get it. But the retinopathy that destroys vision, proliferative retinopathy, is far less common.
Who is at risk of getting retinopathy?
People who keep their blood sugar levels closer to normal are less likely to have retinopathy or will have milder forms.
What are the symptoms of diabetic retinopathy?
Your retina can be badly damaged before you notice any change in vision. Most people with nonproliferative retinopathy have no symptoms. Even with proliferative retinopathy, the more dangerous form, people sometimes have no symptoms until it is too late to treat them. For this reason, you should have your eyes examined regularly by a diabetic eye specialist at Ophthalmic Consultants of the Capital Region.
The earliest sign of diabetic retinopathy is usually the appearance of microaneurysms on the surface of the eye, which look like small, red dots. Although diabetic retinopathy will eventually cause vision problems, vision loss usually doesn’t appear in the early onset of diabetic retinopathy.
I have early diabetic retinopathy. What is the treatment?
If you have nonproliferative diabetic retinopathy, you may not need treatment right away. However, your retinal disease specialist will closely monitor your eyes to determine if and when you need treatment.
It may also be helpful to work with your diabetes doctor to find out if there are any additional steps you can take to improve your diabetes management.
nūretin®
Now available at Ophthalmic Consultants of the Capital Region. nūretin is a specially formulated medical food to delay the onset and/or slow the progression of diabetic retinopathy. If you have diabetes, ask your eye doctor if nūretin is right for you.
I have advanced diabetic retinopathy. What is the treatment?
If you have proliferative diabetic retinopathy, you may need prompt surgical treatment. Surgery often slows or stops the progression of diabetic retinopathy, but it’s not a cure. Because diabetes is a lifelong condition, future retinal damage and vision loss are possible. Even after treatment for diabetic retinopathy, you’ll need regular eye exams. At some point, additional treatment may be recommended.
Depending on the specific problems with your retina, treatment options for advanced diabetic retinopathy may include:
- Focal Laser Treatment
This laser treatment, also known as photocoagulation, can stop or slow the leakage of blood and fluid in the eye. During the procedure, leaks from abnormal blood vessels are treated with laser burns. - Scatter Laser Treatment
This laser treatment, also known as pan-retinal photocoagulation, can shrink the abnormal blood vessels. During the procedure, the areas of the retina away from the macula are treated with scattered laser burns. The burns cause abnormal new blood vessels to shrink and scar. - Vitrectomy
This procedure can be used to remove blood from the middle of the eye (vitreous) as well as any scar tissue that’s tugging on the retina. During the procedure, the retinal disease specialist makes a tiny incision in your eye. Scar tissue and blood in the eye are removed with delicate instruments and replaced with a salt solution, which helps maintain your eye’s normal shape. Sometimes a gas bubble must be placed in the cavity of the eye to help reattach the retina - Anti-VEGF Medication Injections
Your eye doctor at Ophthalmic Consultants of the may suggest injecting an anti-VEGF medication into the eye. Many patients respond well to the use of anti-VEGF medication to stop the progression of diabetic retinopathy. The Anti-VEGF medication works by inhibiting the body’s ability to send the messages for new blood vessel growth.
What are other eye complications diabetes can cause?
Glaucoma
People with diabetes are 40 percent more likely to suffer from glaucoma than people without diabetes. The longer someone has had diabetes, the more common glaucoma is. Risk also increases with age. Click here for more information on glaucoma.
Cataracts
People with diabetes are 60 percent more likely to develop cataracts. People with diabetes also tend to get cataracts at a younger age and have them progress faster. Click here for more information on cataracts.
Macular Edema
The capillary walls in your eyes may lose their ability to control the passage of substances between the blood and the retina. Fluid can leak into the part of the eye where focusing occurs, the macula. When the macula swells with fluid, it creates a condition called macula edema, in which vision blurs and can be lost entirely. Macular edema must be treated, but, fortunately, treatment is usually effective at stopping and sometimes reversing vision loss.
There are two types of treatment for macular edema: focal laser therapy that slows the leakage of fluid, and medications that can be injected into the eye that slow the growth of new blood vessels and reduce the leakage of fluid into the macula.
FIVE CONVENIENT LOCATIONS
Ophthalmic Consultants of the Capital Region has five convenient locations to serve all your eye care needs. No need to travel to the big city. You can find advanced eye care right here in your hometown.
We have offices in:
NEXT STEPS
If you’re experiencing blurred vision, floaters, flashes of light, or have been diagnosed with diabetes, it is important to call us immediately to schedule an appointment. Receiving prompt treatment can be critical to your sight.
Get in touch with us today at our nearest location to you.

